
Pediatric Advanced Life Support (PALS) certification is one of the most critical credentials a healthcare professional can hold. Developed by the American Heart Association in collaboration with the American Academy of Pediatrics, the PALS course equips providers with the systematic approach, clinical algorithms, and hands-on skills needed to recognize and treat critically ill infants and children. Whether you are a pediatric nurse, an emergency medicine physician, a paramedic, or a respiratory therapist, PALS training prepares you for the high-stakes moments when a child's life depends on your ability to act quickly and decisively. This guide covers everything you need to know about PALS certification — from who needs it and what the course covers, to exam preparation strategies and what the 2025 AHA Guidelines mean for pediatric resuscitation.
Who Needs PALS Certification?
PALS certification is intended for healthcare professionals who respond to emergencies involving infants and children, as well as personnel in emergency response, emergency medicine, intensive care, and critical care units who regularly encounter pediatric patients. The American Heart Association specifically recommends PALS for providers whose clinical responsibilities include managing cardiopulmonary arrest, respiratory emergencies, and shock in pediatric patients.
In practice, the following professionals are most commonly required or strongly encouraged to hold current PALS certification:
- Emergency department physicians and nurses — pediatric emergencies can present at any ED, not just children's hospitals
- Pediatric ICU and NICU staff — nurses, respiratory therapists, and physicians managing critically ill children
- Paramedics and EMTs — prehospital providers who may be the first to assess and treat a pediatric patient in the field
- Pediatricians and family medicine physicians — office-based providers who may encounter acute deterioration
- Anesthesiologists and CRNAs — particularly those involved in pediatric surgical cases
- Respiratory therapists — essential team members during pediatric airway emergencies
- Flight nurses and critical care transport teams — providers who manage pediatric patients during interfacility transfers
Many hospitals, ambulance services, and healthcare systems require PALS certification as a condition of employment or credentialing. Even in settings where it is not strictly mandated, PALS training provides a structured framework for managing the unique physiological and anatomical challenges of pediatric emergencies — challenges that differ substantially from adult resuscitation.
Why Pediatric Emergencies Require Specialized Training
Children are not simply small adults. Their airways are anatomically different — shorter, narrower, and more easily obstructed. Their cardiovascular physiology responds differently to illness and injury. And the causes of cardiac arrest in children differ fundamentally from those in adults: while adult cardiac arrest is most often caused by primary cardiac events (ventricular fibrillation or tachycardia), pediatric cardiac arrest is overwhelmingly the result of progressive respiratory failure or circulatory shock that goes unrecognized or untreated.
This distinction is central to the PALS philosophy. The course emphasizes early recognition and intervention — identifying the child who is deteriorating before cardiac arrest occurs, rather than focusing solely on resuscitation after the heart has stopped. Studies consistently show that outcomes from pediatric cardiac arrest are significantly better when the underlying cause (respiratory distress, shock, arrhythmia) is identified and treated early in its progression.
What the PALS Course Covers
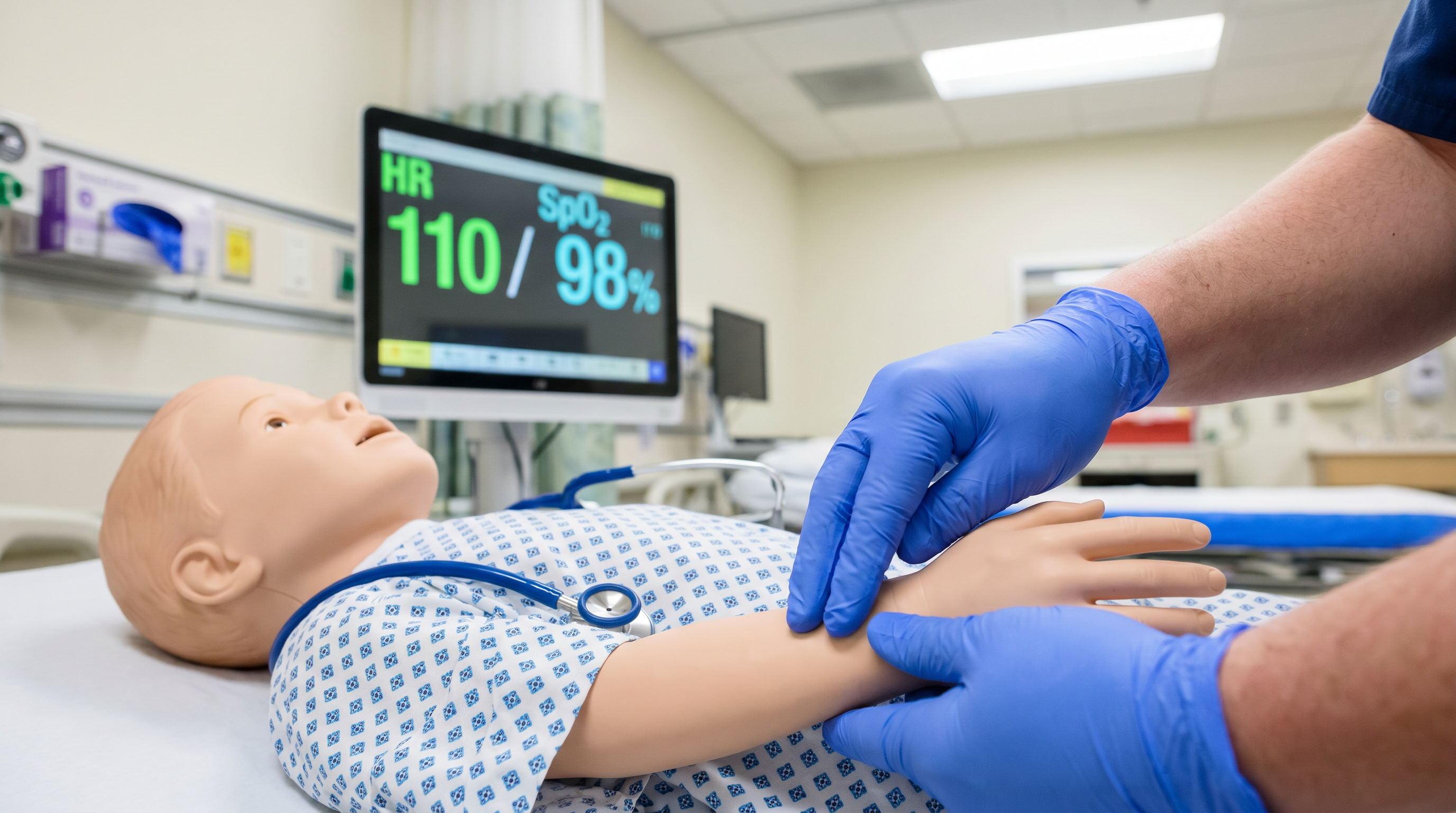
The AHA PALS Provider Course is a comprehensive training program that combines didactic instruction, interactive case discussions, and hands-on skills practice. The course uses a systematic approach to teach providers how to assess and manage pediatric patients in emergency situations, progressing from initial assessment through definitive treatment.
The PALS Systematic Approach
At the heart of the PALS course is the Systematic Approach Algorithm, which provides a structured framework for evaluating every critically ill or injured child. The approach begins with an initial impression — a rapid, visual assessment of the child's appearance, work of breathing, and circulation (the Pediatric Assessment Triangle). This is followed by a primary assessment evaluating airway, breathing, circulation, disability (neurological status), and exposure, and then a secondary assessment that includes a focused history and detailed physical examination.
This systematic approach ensures that providers do not skip critical steps under pressure and that life-threatening conditions are identified in the correct order of priority. The course reinforces this framework through repeated practice across multiple clinical scenarios.
Core Clinical Content
The PALS course covers four major categories of pediatric emergencies, each with specific recognition criteria, treatment algorithms, and management strategies:
Respiratory Emergencies: The course teaches providers to distinguish between upper airway obstruction (croup, foreign body, anaphylaxis), lower airway obstruction (asthma, bronchiolitis), lung tissue disease (pneumonia, pulmonary edema), and disordered control of breathing. Each category has specific signs, symptoms, and treatment pathways. Providers learn airway management techniques including bag-valve-mask ventilation, oropharyngeal and nasopharyngeal airways, and the principles of advanced airway placement.
Shock: PALS covers the four types of shock — hypovolemic, distributive, cardiogenic, and obstructive — with emphasis on early recognition through assessment of heart rate, blood pressure, capillary refill, skin color, and mental status. Providers learn fluid resuscitation strategies, vasopressor and inotrope selection, and the critical importance of reassessment after each intervention.
Cardiac Arrhythmias: The course covers recognition and management of pediatric bradycardia (symptomatic and asymptomatic), tachycardia (supraventricular tachycardia, ventricular tachycardia), and cardiac arrest rhythms (ventricular fibrillation, pulseless ventricular tachycardia, asystole, pulseless electrical activity). Providers learn the appropriate use of vagal maneuvers, adenosine, amiodarone, epinephrine, and electrical therapy (defibrillation and cardioversion).
Cardiac Arrest: The course integrates all of the above into the management of pediatric cardiac arrest, emphasizing high-quality CPR, early defibrillation for shockable rhythms, appropriate medication administration, and identification and treatment of reversible causes (the H's and T's).
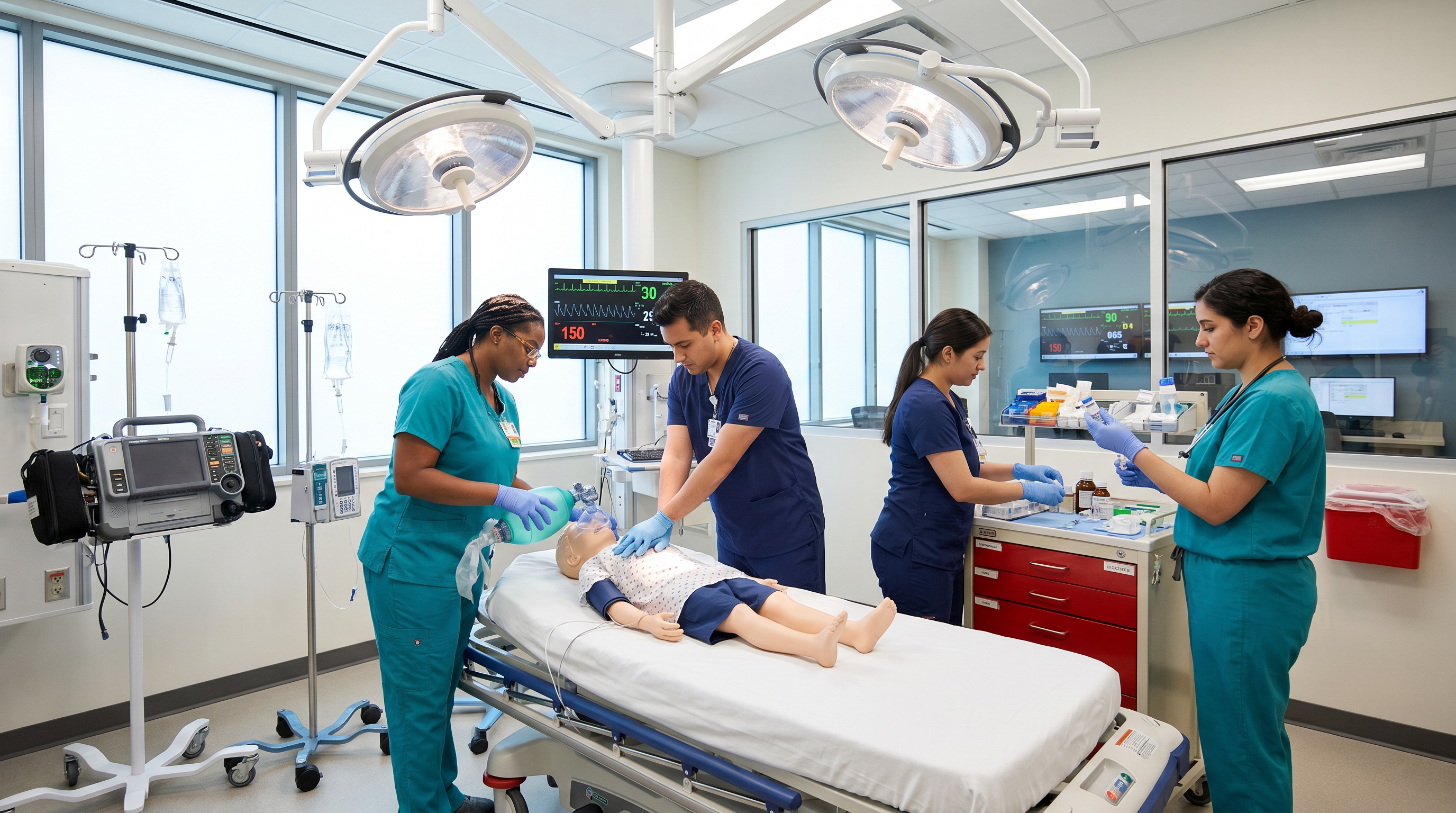
Team Dynamics and Communication
Effective pediatric resuscitation requires coordinated teamwork. The PALS course dedicates significant time to team dynamics — clear role assignment, closed-loop communication, mutual respect, and constructive intervention when errors are observed. Providers practice leading and participating in resuscitation teams during simulated scenarios, building the communication skills that are essential when seconds count.
Course Format and Duration
The AHA offers several PALS course formats to accommodate different learning preferences and schedules. All formats teach the same science-based content and result in the same AHA PALS Provider Course Completion eCard, valid for two years.
| Format | Duration | Description |
|---|---|---|
| ILT Full Course | ~12.5 hours (with breaks) | Fully instructor-led classroom course covering all content, skills practice, and testing |
| ILT Update Course | ~8.75 hours (with breaks) | Renewal course for currently certified providers; reviews updates and tests proficiency |
| HeartCode PALS (Blended) | Online (varies) + ~5.5 hours hands-on | Self-paced online learning with adaptive algorithm, followed by instructor-led skills session |
| HeartCode Complete | Varies by experience | Fully self-paced online learning plus skills verification at a CPR Verification Station |
At EMIC, we offer instructor-led PALS courses with flexible scheduling, including the option for 1:1 instruction. Our personalized approach allows many students to complete the course more efficiently than the standard timeline, without sacrificing the depth of learning or hands-on practice that makes PALS training effective.
The PALS Exam: What to Expect
PALS certification requires passing both a written (cognitive) exam and a skills evaluation. Understanding the format and expectations for each component helps reduce test anxiety and allows you to focus your preparation effectively.
Written Exam
The PALS written exam consists of 50 multiple-choice questions covering the full scope of course content — systematic assessment, respiratory emergencies, shock management, cardiac arrhythmias, cardiac arrest algorithms, pharmacology, and team dynamics. A minimum score of 84% is required to pass. Questions are scenario-based, presenting clinical situations and asking you to identify the correct assessment finding, intervention, medication, or next step.
The exam tests your ability to apply knowledge rather than simply recall facts. For example, rather than asking "What is the dose of epinephrine?", a question might present a clinical scenario of a child in pulseless electrical activity and ask you to identify the appropriate next intervention in the algorithm. This application-based format rewards understanding over memorization.
Skills Evaluation
The skills evaluation assesses your ability to perform high-quality CPR, manage a pediatric airway, and lead or participate in a simulated resuscitation scenario. You will demonstrate competency in infant and child CPR technique, bag-valve-mask ventilation, and the management of at least one simulated case (such as a child in respiratory distress progressing to arrest, or a child presenting with an unstable arrhythmia). Instructors evaluate your performance using standardized checklists, and a minimum score of 80% is required.
The most common areas where students struggle during the skills evaluation are maintaining proper compression depth and rate during infant CPR, delivering effective bag-valve-mask ventilations with visible chest rise, and verbalizing the correct algorithm steps under the pressure of a simulated scenario. Practicing these skills repeatedly during the course — and arriving with a solid understanding of the algorithms — significantly improves your chances of passing on the first attempt.
How to Prepare for Your PALS Course
Before the Course
Thorough preparation before arriving at your PALS course makes a significant difference in both your learning experience and your likelihood of passing. The AHA recommends completing all pre-course work, which typically includes reading the PALS Provider Manual and completing any assigned online modules. Focus your study on the following high-yield areas:
- PALS algorithms: Familiarize yourself with the Cardiac Arrest, Bradycardia, and Tachycardia algorithms — know the decision points and medication sequences
- Pediatric pharmacology: Review key medications (epinephrine, amiodarone, adenosine, atropine) including weight-based dosing, routes of administration, and indications
- Rhythm recognition: Practice identifying normal sinus rhythm, sinus tachycardia, SVT, ventricular tachycardia, ventricular fibrillation, asystole, and PEA on pediatric rhythm strips
- Pediatric assessment: Understand the Pediatric Assessment Triangle and the primary/secondary assessment sequence
- Age-specific vital signs: Know the normal ranges for heart rate, respiratory rate, and blood pressure by age group
During the Course
Active participation is the single most important factor in getting the most from your PALS course. Volunteer to lead scenarios during practice stations, ask questions when concepts are unclear, and take every opportunity to practice hands-on skills. The course is designed as a learning environment — instructors expect questions and provide coaching throughout. Students who engage actively during practice scenarios consistently perform better during the final skills evaluation than those who observe passively.
2025 AHA Guidelines: What Changed for PALS
The 2025 American Heart Association Guidelines for CPR and Emergency Cardiovascular Care, published in October 2025, include significant updates to pediatric advanced life support. These guidelines, codeveloped with the American Academy of Pediatrics, represent a comprehensive revision of the evidence base for pediatric resuscitation. Key updates include:
Physiology-Directed Resuscitation: The 2025 guidelines explicitly elevate the concept of physiology-directed resuscitation — a shift from purely protocol-driven approaches toward using real-time physiological data (such as end-tidal CO2, arterial blood pressure, and oxygen saturation) to guide resuscitation decisions. This represents a significant conceptual advancement, encouraging providers to treat the patient's physiology rather than rigidly following a one-size-fits-all algorithm.
Updated Algorithms: The pediatric cardiac arrest, bradycardia, and tachycardia algorithms have been refined to incorporate new evidence regarding medication timing, energy dosing for defibrillation, and the role of extracorporeal CPR (ECPR) in select populations. The systematic approach algorithm has also been updated to reflect current best practices in pediatric assessment.
Airway Management: The guidelines provide updated recommendations on airway management strategies, including the use of video laryngoscopy, cuffed endotracheal tubes in infants and children, and the timing of advanced airway placement relative to other resuscitation interventions.
Post-Cardiac Arrest Care: Enhanced emphasis on post-resuscitation care, including targeted temperature management, hemodynamic monitoring, and neuroprognostication in children following return of spontaneous circulation (ROSC).
All current PALS courses offered through AHA Training Centers, including those at EMIC, are updated to reflect the 2025 Guidelines. If you were last certified under the 2020 Guidelines, your renewal course will cover these important updates.
Certification and Renewal
Upon successful completion of both the written exam and skills evaluation, you receive an AHA PALS Provider Course Completion eCard, valid for two years. At EMIC, we issue eCards the same day, so you leave your course with your credential ready to submit to your employer or credentialing body.
Renewal (recertification) is required every two years. If your certification is current or has been expired for fewer than 30 days, you are eligible for the PALS Update Course, which is shorter than the full provider course and focuses on reviewing skills, testing proficiency, and covering any guideline updates. If your certification has been expired for longer, you will need to complete the full PALS Provider Course again.
The AHA recommends that providers maintain their skills between certification cycles through regular practice, participation in simulation exercises, and review of algorithm cards. Skills decay is well-documented in resuscitation education research — providers who practice regularly retain proficiency far better than those who only review material immediately before renewal.
Why Choose EMIC for PALS Training
At EMIC, our PALS courses are taught by experienced healthcare professionals who bring real-world pediatric emergency experience to every class. We maintain small class sizes — and offer 1:1 instruction for those who prefer it — ensuring that every student receives individualized attention during skills practice and scenario-based learning.
Our approach to PALS training goes beyond checking a box. We focus on building genuine clinical confidence, not just passing a test. Our instructors create a supportive learning environment where questions are encouraged, mistakes are treated as learning opportunities, and every student leaves feeling prepared to manage a real pediatric emergency.
The EMIC Advantage
- Flexible scheduling: Courses available 7 days a week with morning, afternoon, and evening options
- 1:1 instruction available: Personalized training that adapts to your pace and learning style
- Written or electronic exams: Choose the format that works best for you
- Comprehensive exam remediation: If you don't pass on the first attempt, we provide detailed analysis and targeted support
- Same-day eCard issuance: Leave with your certification ready to submit
- Lowest rates in New York State: Competitive pricing without compromising quality
- Custom study guides: Tailored materials for students who need additional support
Whether you are certifying for the first time or renewing an existing credential, EMIC provides the training, support, and flexibility you need to earn your PALS certification with confidence. Contact us today to schedule your course.
References
- American Heart Association. (2025). Part 8: Pediatric Advanced Life Support: 2025 American Heart Association Guidelines for CPR and Emergency Cardiovascular Care. Circulation, 152(suppl 2). ahajournals.org
- American Heart Association. (2025). PALS Course Options. CPR & First Aid. cpr.heart.org
- American Heart Association. (2025). Highlights of the 2025 American Heart Association Guidelines for CPR and Emergency Cardiovascular Care. cpr.heart.org (PDF)
- American Heart Association & American Academy of Pediatrics. (2025). Part 6: Pediatric Basic Life Support: 2025 American Heart Association Guidelines. Circulation, 152(suppl 2). ahajournals.org
- Topjian, A. A., et al. (2020). Part 4: Pediatric Basic and Advanced Life Support: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation, 142(16_suppl_2), S469–S523. ahajournals.org
